Nursing Simulation Lab

So…you are thinking about incorporating a Simulation Lab into your Nursing program. Perhaps you have visited a few facilities at peer institutions to talk with colleagues and determine what you like and what you don’t like, researched on-line to see how others are using these spaces. You begin to envision how a facility will support your program, how your faculty will teach, and what YOUR Sims Lab will look like and function based on these experiences.
Before you embark on this journey, here are a few things worthy of your consideration. In the world of maximizing assignable space in Higher Education, numbers matter. Questions to ask yourself and your colleagues include…
- How do we integrate the Simulation Lab into our academic program while considering the make-up of our faculty?
- How many students are currently enrolled in the Nursing Program and what are the projections for future enrollment?
- What type of clinical environment are we trying to simulate…patient room, examination / treatment room, trauma room, etc. and what level of simulation fidelity will we be able to afford?
- How many SIMS rooms do we need? And how many support spaces such as control rooms, debriefing rooms, manikin & medical equipment storage rooms do we need?
- Is this an opportunity to upgrade the nursing program’s facilities…how many dedicated nursing classrooms, computer labs, study lounges, and faculty offices do we need?
Program Impact

Penn State Altoona | Aaron Building Nursing Simulation and Skills Laboratory
This consideration is directly grounded in your faculty and the current (and future) pedagogical approach. A Johns Hopkins School of Nursing study published in 2014 suggests that applying simulation to the educational process provides relief to the struggle of finding clinical placements while achieving equivalent clinical training results. But, while the data supports this as valid training approach, it does not address acceptance of the practice at the faculty level.
Critical to implementing a simulation component into your curriculum is building consensus amongst your faculty and altering your curriculum to integrate simulation as part of the instructional process. While time will reduce the skeptics as the next generation of instructors who grew up with technology become instructors, care should be exercised to consider this when projecting student throughput expectations.
Vital to a successful simulation curriculum is understanding how faculty will use the space, not only to simulate clinical situations but the crucial debriefing session. Time allocated and number of rooms for debriefing of the clinical simulation will determine the throughput capacity.
It is no secret that there aren’t enough Nursing Faculty to handle the increasing enrollments. Consider the following statistics.
- A total of 1,715 faculty vacancies were identified in a survey of 872 nursing schools with baccalaureate and/or graduate programs across the country. Besides the vacancies, schools cited the need to create an additional 138 faculty positions to accommodate student demand. The data show a national nurse faculty vacancy rate of 7.9%. Most of the vacancies (90.7%) were faculty positions requiring or preferring a doctoral degree.
- The average ages of PhD-prepared nurse faculty holding the ranks of professor, associate professor, and assistant professor were 62.4, 57.2, and 51.2 years, respectively.
- For master's degree-prepared nurse faculty, the average ages for professors, associate professors, and assistant professors were 55.5, 56.4, and 50.6 years, respectively.
Sources
1 AACN Special Survey on Vacant Faculty Positions, October 2018.
2,3 AACN's report on 2016-2017 Salaries of Instructional and Administrative Nursing Faculty
One of two things need to happen. More nursing faculty must matriculate or integrating a Simulation Lab to increase throughput is needed.
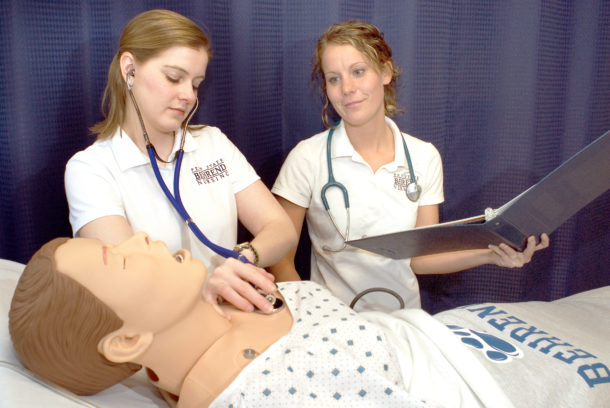
Penn State Behrend | Nursing Sims Lab
Student Enrollment
Obviously current enrollment is an important factor. Considering enrollment projections is critical. While demand for nursing graduates continues to rise, teaching spaces need to be adaptable to fluctuations in enrollment levels. A realistic assessment of student enrollment projections is critical to rightsizing your Simulation Lab.
According to the American Association of Colleges of Nursing there are some sobering statistics related to Nursing School Capacity/Faculty Shortage.
- In 2018, 75,000 qualified nursing applicants turned away from BSN and graduate programs.
- AACN forecasts 1/3 of nursing faculty will retire by 2025.
Sources
1,2 AACN Fact Sheet: Nursing Faculty Shortage April 2019
The clinical simulations desired help to define the space type. This also helps to define the equipment required for simulation. Medical gases, medical lighting, medical equipment, hand washing stations, etc. will be configured based on the clinical simulation. While patient rooms, evaluation and treatment rooms, and trauma spaces are different in certain aspects, designing a flexible space to accommodate evolution of the program and teaching methodology is wise.
The fidelity of the simulations you are implementing needs to be assessed. The higher the fidelity the more realistic the simulation is. The number of elements and factors introduced to the simulation helps to define the fidelity of the simulation. In medical field simulations, low fidelity activities done repeatedly often help to build the basic skill set to accomplish tasks necessary in a clinical situation. Increasing the fidelity of the simulations over time allows the student to build on tasks previously learned.

Penn State Behrend | Nursing Sims Lab Control Room
How Many … Sims Space?
This requires some critical thinking on how you intend to integrate simulation into your program. The bed to observation room ratio is dependent on the expected throughput. Thought should be centered around the number of students (and projected enrollment), active faculty, and anticipated pedagogy.
According to Johns Hopkins University, a 1:1 ratio of simulation rooms to debriefing rooms is desirable to run a course. This allows back and forth use of simulation and debriefing rooms for the duration of a class. In real-life situations, debriefing rooms in critical care suites also can be used as family consult rooms.
The types of clinical simulation you are integrating into your program must be considered. The spaces that support simulation include patient rooms, trauma spaces, examination and treatment rooms, all of which have different configuration and equipment requirements. While creating flexible spaces allows for fluctuations in enrollment and curriculum evolution, how many spaces with corresponding control and observation rooms needs to be quantified.
How Many...Nursing Program Space?
Improvements to the Program’s facilities are often included when Sims Labs are implemented. The thinking is, "let’s do this at one time." It’s less expensive in the long run (as compared to several smaller projects). Also, it minimizes the disruption that happens during construction. If you are fortunate to have the opportunity to improve your overall Program facilities, considering how the Sims Lab will impact your overall pedagogy as you implement simulations into the curriculum.
Support Spaces
One of the most often overlooked and undersized support space is storage. Consider how equipment and supplies will be stored. Also, will storage be required for the students to store their backpacks and coats while in the lab. Consider a mix of locked and open storage to accommodate varying needs.
Additionally, the renovation of existing space for a simulation lab extends to other areas. If you have the opportunity augment your faculty offices, kitchen, conference rooms, etc., consider configuring the spaces to support the programs and sims labs goal while avoiding disturbing the instruction taking place in the SIMS Lab.
Changes to your curriculum through Sims Lab integration will help to define how many dedicated nursing classrooms, computer labs, study lounges, and faculty offices you will need.
Consider what is going to be taught in the simulation lab that was taught in the traditional classroom and/or through clinical placements. Does this impact the number of dedicated classrooms that you need?
Computer labs are often spaces that synthesize learning and socialization. Walk around your campus and visit other computer labs on your campus at varying times of the day. This will give you a feel as to how students are using the spaces.
Study lounges are also spaces where students study and socialize. Flexibility is key here to accommodate both group and individual study needs.
Faculty offices should be flexible as well. Not only to adjust for the number of faculty but to consider the office needs of younger faculty that often requires spaces that are technology rich as opposed to paper heavy.
Summary
Implementing a Sims Lab into your curriculum is change. And, we all know that change can be difficult. Managing the change by focusing on the expected outcomes is prudent and will help to create a staff that flourishes throughout the process.
Success should be measured on the impact the Sims Lab has on the Program and your students. Hiring a professional that helps you and your team craft the vision for program improvements is critical to success. Good luck on your journey!


